(Código CIE-9-MC: 348.0)
Quiste aracnoideos, también conocidos como quistes leptomeníngeos.
Los quistes aracnoideos (QA) son estructuras patológicas de características benignas que podríamos definir como cavidades rellenas de líquido claro similar al líquido cefalorraquídeo (LCR), contenido dentro de una membrana indistinguible histológicamente de la aracnoides sana.
Se producen durante la división de la aracnoides.
La hipótesis más aceptada habla de alteraciones en la separación del endomenix en el tercer trimestre del período neonatal. El endomenix es una membrana de tejido mesenquimal que rodea al tubo neural. En el tercer trimestre, cuando se rompe el techo del cuarto ventrículo, ondas de presión de LCR fluyen a través de ella, la disecan en dos capas y dan lugar a la piamadre, la aracnoides y el espacio subaracnoideo. Las alteraciones de este mecanismo podrían dar lugar a la formación de cavidades separadas que, en su crecimiento, formarían quistes.
Otras hipótesis planteadas hablan de que son secundarios a hipoplasias encefálicas focales, en las que ocupan el espacio cedido o que se producen por alteraciones de la secreción de sustancias del espacio subaracnoideo al sistema venoso. Asimismo, para explicar el posterior crecimiento del quiste se han planteado diversas teorías; entre ellas, la más aceptada, porque existen casos en los que se ha podido demostrar in vivo, es la formación de mecanismos valvulares . También se han descrito en la literatura algunos casos de quistes relacionados con infecciones meníngeas y traumatismos, llamados secundarios, en contraposición con aquellos de los que se desconoce la causa y se sospecha de malformación congénita, y que se denominan primarios.
Realmente pues son quistes intraaracnoideos. Cuando se diagnosticaban a nivel de fosa media se les llamó » síndrome » de agenesia de lóbulo temporal. (Este término es ahora obsoleto).
Otros son los producidos por traumatismos.
Una fractura lineal simple, sin complicaciones inmediatas, puede originar el desarrollo de un quiste aracnoideo, de ahí que se deba mantener un correcto seguimiento de la evolución de la consolidación de la fractura y una alerta etiológica ante la aparición de clínica neurológica.
Incidencia
Constituyen un diagnóstico típico de la infancia, sobre todo en los dos primeros años de vida, donde representan aproximadamente el 1% de las lesiones expansivas intracraneales. Las localizaciones más frecuentes encontradas en diversas series son la cisura de Silvio y la fosa posterior.
5 por 1000 en autopsias.son lesiones características de la infancia, ligeramente más frecuentes en varones.
También se encuentran a nivel espinal aunque son raros.
Localización
- Cisura de silvio 49%
- APC 11%
- Supracolicular 10%
- Vermiano 9%
- Selar y supraselar 9%
- Interhemisférico 5%
- Convexidad 4%
- Clivus 3%
Tipos histológicos
Los quistes simples: Línea celular que parecen ser capaz de la secreción de LCR. Los quistes de la fosa media parecen ser exclusivamente de este tipo
Los quistes complejos que también puede contener neuroglia, epéndimo, y otros tipos de tejido.
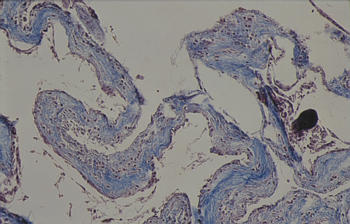
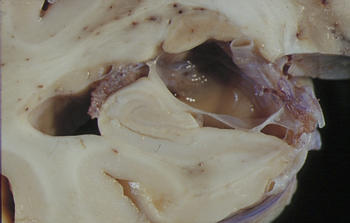
Presentación Clínica
La sintomatología es variable según que parte del sistema nervioso central comprima, lo más llamativo son síntomas focales con signos de hipertensión intracraneal, como son cefalea (dolor de cabeza), hemiparesia,diplopia (visión doble), irritabilidad, cambios de carácter, apatía (carencia de emociones), y deterioro del rendimiento intelectual.
Fosa Media Supraselares con hidrocefalia difusas supra o infratentoriales con hidrocefalia
Epilepsia,cefalea,hemiparesia HTE,Craneomegalia,desarrollo tardío,pérdida de agudeza visual,pubertad precoz HTE,craneomegalia,desarrollo tardío
La mayoría de los quistes son sintomáticos en la infancia.
Se pueden diagnosticar a través de la presencia de:
- Síntomas de aumento de la presión intracraneal (Cefalea, náuseas…)
- Epilepsia.
- Deterioro súbito: debido a la hemorragia (en quiste o subdural): los quistes de fosa medial son proclives a hemorragia debido a la mayor posibilidad de ruptura de venas puente; debido a la ruptura del quiste
- Protrusión en el cráneo
- Signos neurológicos focales.
- Hallazgo incidental.
- Hidrocefalia (Probablemente debido a la compresión del tercer ventrículo)
- Síntomas endocrinos: ocurren en un 60%. Incluye la pubertad precoz.
- Deterioro visual
- En fosa posterior suelen producir síntomas inespecíficos como hipoacusia y acúfenos aveces incluso dificiles de distinguir de una enfermedad de Meniere y lo más característico suelen ser ataxias cerebelosas.
Diagnóstico
Se diagnostican en primera instancia por TAC.
El método ideal RNM y secuencias de difusión (planteará mejor el diagnóstico diferencial con los quistes epidermoides o neoplásicos hemangioblastomas).
Diagnóstico diferencial
- Astrocitomas quísticos.
- Cisterna magna grande
- Quiste hidatídico – Cisticercosis
- Infarto crebral antiguo
- Porencefalia.
- Cavum de línea media.
Tratamiento
Se recomienda tratar solo los que producen síntomas independientemente de la localización y tamaño. Aún el tratamiento es muy controvertido.
Entre las opciones terapéuticas tenemos la fenestración endoscópica o por craneotomía hacia el ventrículo o espacio subaracnoideo y la implantación de una derivación.
Probablemente el mejor tratamiento consista en la derivación del quiste a peritoneo.
Procedimiento Ventajas Desventajas
Punción aspiración- trépano Fácil y rápido Recurrencia
Craneotomía con excisión de la pared quísticay fenestración a espacio subaracnoideo o ventricular Permite inspección del quiste y estructuras vasculares. Evita en algunos caso la derivación permanente. Reacumulación posible y más invasivo.
Derivación cistoperitoneal Procedimiento simple Dependencia Shunt y riesgos de portar Shunt.
Dr. J. Sales Llopis
Servicio de Neurocirugía del Hospital General Universitario de Alicante.
Para consultar:
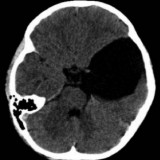








Buenas Tardes tengo 34 años y hace 2 meses empecé a sufrir de fuertes dolores de cabeza, cansancio, cambios de carácter, por momentos veo borroso o veo doble, mareos y pérdidas de equilibrio. Me hicieron una tomografía y salió que tengo quistes aracnoideos en ambas regiones temporales basales. Cada cierto tiempo me da estos síntomas, pero los dolores de cabeza duran alrededor de casi 2 semanas y luego me calman. Por favor su apoyo esto es operable y que consecuencias hay posteriormente. A la espera de sus comentarios. Gracias.